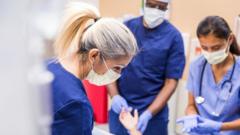
The air in the triage bay doesn't smell like medicine anymore. It smells like unwashed bodies, cold coffee, and the sharp, metallic tang of adrenaline that has stayed in the system too long.
Sarah is a senior registrar. She has spent twelve years learning how to save lives, but lately, her job feels less like medicine and more like a cruel math problem. At 3:00 AM, the department isn't just full; it’s over-saturated. Every cubicle is occupied. The "corridor queue" has stretched past the double doors and into the ambulance bay. For a different view, read: this related article.
Then the red phone rings.
Two ambulances are three minutes out. The first carries a sixty-four-year-old man in cardiac arrest—active CPR in progress. The second carries a twenty-two-year-old woman involved in a high-speed collision; she’s hemodynamically unstable, which is a clinical way of saying she is bleeding out internally and her heart is struggling to keep up. Further coverage on this trend has been published by Medical News Today.
In a functional world, Sarah would have two resuscitation teams and two empty trauma bays. Tonight, she has neither. She has one bay currently occupied by a patient who isn't stable enough to move, and one nursing team that hasn't had a bathroom break in nine hours.
This is the reality of modern emergency medicine. It isn't a shortage of Band-Aids or high-tech scanners. It is the systematic collapse of a safety net that has been stretched until the fibers are snapping one by one. Doctors are no longer just treating the sick. They are being forced to choose who stays sickest the longest.
The Weight of the Invisible Wait
When we talk about "waiting times," the brain tends to conjure images of a DMV office or a slow line at a grocery store. We think of boredom. We think of inconvenience.
In an Emergency Department, a wait is a biological process.
Consider a hypothetical patient we’ll call Arthur. Arthur is eighty. He has a mild infection and a bit of confusion. In a healthy hospital system, Arthur is seen within an hour, given IV fluids and antibiotics, and moved to a ward bed. But today, the wards are full of "medically fit" patients who cannot be discharged because there is no social care available to catch them.
So, Arthur sits on a hard plastic chair in the waiting room. Then he’s moved to a trolley in a hallway.
Six hours pass. His infection worsens. Twelve hours pass. He becomes delirious. Eighteen hours pass. Because he is on a trolley and not a specialized hospital bed, his skin begins to break down. By the time Sarah can finally find a moment to treat him, Arthur isn't just a man with an infection anymore. He is a man with a pressure sore, acute delirium, and a skyrocketing risk of hospital-acquired pneumonia.
The "wait" changed his clinical outcome. It turned a three-day stay into a three-week struggle. This is the "invisible stake" that doesn't show up on a spreadsheet. Every hour a patient spends on a trolley in a corridor increases the statistical likelihood of their death within thirty days. It is a slow-motion catastrophe, measured in minutes but paid for in lives.
The Triage of the Soul
Triage was originally a battlefield concept. It was designed for Napoleonic wars and muddy trenches, a way to sort the "salvageable" from those who would die regardless of intervention. It was never intended to be the permanent operating state of a civil society’s healthcare system.
Yet, here we are.
Doctors are now practicing "corridor triage." This isn't about who goes first; it’s about who is least likely to die in the next ten minutes if ignored. It creates a moral injury that stays with a clinician long after their shift ends.
Sarah looks at the two incoming ambulances. She has to make a choice. If she moves the unstable patient out of the only available trauma bay to make room for the cardiac arrest, she might kill the person she’s currently trying to save. If she leaves them there, the man in the ambulance has zero chance of survival.
She is playing God with a hand tied behind her back.
This pressure creates a specific kind of exhaustion. It isn't the "good" tired that comes from a hard day's work. It is a corrosive, soul-deep fatigue. When you are forced to provide suboptimal care day after day—not because you lack the skill, but because the system lacks the space—your professional identity begins to erode. You stop being a healer and start being a gatekeeper.
The Myth of the "Inappropriate" Visit
There is a common narrative that emergency departments are failing because people show up with "stubborn coughs" or "broken fingernails." It’s a convenient story. It shifts the blame from the policymakers to the public.
It is also largely a myth.
While there will always be people who use the ER for minor ailments, they aren't the ones causing the gridlock. A person with a cough takes five minutes to assess and discharge. They don't take up a bed. They don't require a six-person trauma team.
The gridlock is caused by "exit block."
Think of a hospital like a giant plumbing system. The Emergency Department is the intake pipe. The hospital wards are the main tank. Social care—nursing homes, home-visit carers, rehabilitation centers—is the drainage system.
Right now, the drainage system is backed up.
Because we have stripped the funding from social care, elderly and vulnerable patients have nowhere to go once their acute medical crisis is over. They stay in the "tank." The tank fills up. Eventually, the water backs up all the way to the intake pipe.
When you see an ambulance queue outside a hospital, you aren't looking at a "busy" ER. You are looking at a hospital that is physically full of people who shouldn't be there, preventing people who should be there from getting through the door.
The Arithmetic of Human Suffering
Data tells us that for every eighty-two patients who wait more than six to eight hours in the ER, there is one "excess" death.
One.
In a large hospital, that can mean dozens of deaths per year that were entirely preventable. These aren't people who died from their illness. They are people who died from the timing of their illness.
If a plane crashed every month due to preventable mechanical failure, the industry would be grounded. There would be an international outcry. But because these deaths happen one by one, behind privacy curtains or in the back of ambulances, they remain abstract. They are "statistical outliers" rather than tragedies.
We have become accustomed to the "winter crisis," as if the cold weather is some unpredictable, sentient enemy. But the crisis is no longer seasonal. It is perennial. It is July, and the trolleys are still in the hallways. It is September, and the red phones are still ringing for beds that don't exist.
The Breaking Point
Back in the bay, Sarah makes her call.
She directs the cardiac arrest to a temporary spot in the corridor, knowing the chances are slim. She keeps the trauma bay for the young woman who is bleeding out, because the math of survival says that is where the resources will do the most good.
She works. Her team works. They move with a frantic, practiced grace, stepping over bags and dodging equipment. They save the woman. They lose the man.
Later, in the quiet of the locker room, Sarah wonders if the man would have lived if he’d arrived five years ago. Or even two. She wonders if his family knows that his "sudden" death was facilitated by a lack of floor space.
She knows she will go home, sleep for four hours, and come back to do it again. But she also knows that the line she is holding—the red line between order and chaos—is getting thinner every night.
The public sees the "Wait Time" clock in the lobby and sighs with frustration. They don't see the doctors in the back, staring at a list of names and trying to decide which life-threatening condition is the most "urgent." They don't see the silent calculations of risk, the whispered apologies to patients in hallways, or the crushing weight of the impossible coin toss.
We have built a system that relies on the heroism of individuals to compensate for the failure of the infrastructure. But heroism is a finite resource. You can only ask people to do the impossible for so long before they simply stop.
And when the heroes leave, all that remains is the red phone, ringing in an empty room.